Birth Asphyxia MRI (BAMRI)
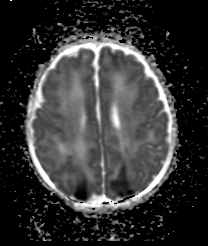 The Birth Asphyxia MRI (BAMRI) project has been ongoing since 1993. The goal was to see how sensitive MRI was in assessing brain injury of babies who had encephalopathy (abnormal neurological exam, seizures, abnormal blood gases) in the neonatal period. We saw that brain injury occurred in certain patterns and were able to conclude that those patterns were associated with specific types of injury. Some types of injuries resulted in damage to areas with high energy demands (brain stem, thalamus, sensorimotor pathways), while others resulted in damage to regions that got less blood flow when blood pressure went down or the heart didn’t contract forcefully. Some babies had damage to the entire brain, presumably due to a long period with essentially no flow to the brain. Still others, had very localized areas of injury, which we call a “stroke” or an infarct. By looking at these patterns of injury and correlating them with outcomes when the babies came back for follow-up neurodevelopmental examinations, our team was able to predict reasonably well what outcome would be based upon the initial MRI.
The Birth Asphyxia MRI (BAMRI) project has been ongoing since 1993. The goal was to see how sensitive MRI was in assessing brain injury of babies who had encephalopathy (abnormal neurological exam, seizures, abnormal blood gases) in the neonatal period. We saw that brain injury occurred in certain patterns and were able to conclude that those patterns were associated with specific types of injury. Some types of injuries resulted in damage to areas with high energy demands (brain stem, thalamus, sensorimotor pathways), while others resulted in damage to regions that got less blood flow when blood pressure went down or the heart didn’t contract forcefully. Some babies had damage to the entire brain, presumably due to a long period with essentially no flow to the brain. Still others, had very localized areas of injury, which we call a “stroke” or an infarct. By looking at these patterns of injury and correlating them with outcomes when the babies came back for follow-up neurodevelopmental examinations, our team was able to predict reasonably well what outcome would be based upon the initial MRI.
As time passed, we got additional tools to use on the MRI and more powerful MRIs; these allowed us to do new and better examinations of the babies’ brains. Proton MR spectroscopy (MRS) allowed us to look at effects of the injury on specific chemicals in the brain. Diffusion weighted MR imaging (DWI), which looks at water motion in the brain, could show smaller areas of injury at earlier times and could be quantified to see how bad the injury was in different locations. Even more important, MRS and DWI showed that the injury in the brain rapidly changed over the first few days; it got much worse between day 1 and day 4. This finding was very important, because it taught us that early intervention might reduce the severity of brain injury. This discovery led to the trial of therapeutic hypothermia (TH, also called “brain cooling”). Recent studies have shown that brain cooling significantly reduces brain injury in some newborns, particularly those with injury to the areas with high energy demands when the injury is not very severe. We think that the babies who do not respond well to TH have a different kind of injury, which has progressed beyond the stage where TH is effective. Different therapies are now being formulated and will be used in upcoming trials to see if they are effective.
Overall, the prognosis for newborn babies with encephalopathy has improved greatly over the past 20 years, and the results of BAMRI have contributed significantly to that improvement!
