Hereditary Hemorrhagic Telangiectasia (HHT)
Hereditary Hemorrhagic Telangiectasia (HHT) is a genetic disorder of the blood vessels which affects approximately one in 5,000 people. The disorder is also referred to as Osler-Weber-Rendu Syndrome. HHT is caused by a mutation in one of several HHT-associated genes. HHT is autosomal dominant, which means that if one of your parents or a sibling has HHT, there is a 1 in 2 chance (50%) that you will have HHT.
The HHT Center of Excellence at UCSF is the only location in Northern California that specializes in the diagnosis and treatment of this disorder.


About HHT
HHT genetic mutations lead to development of abnormal blood vessels that tend to be very fragile and can bleed. An abnormal blood vessel that involves a small blood vessel is called a telangiectasia and most commonly occurs on the face, hands, fingers, and the lining of the nose and mouth. The telangiectasias on the lining of the nose cause recurrent nosebleeds, the most common symptom of HHT. Telangiectasias can also occur in the digestive tract, particularly in the stomach and small bowel.
An abnormal blood vessel that involves a larger blood vessel is called an arteriovenous malformation (AVM). AVMs can occur in one or more organs such as the brain, lungs, and liver which can lead to serious complications as discussed below. Screening tests are available to detect AVMs. If discovered, there are multiple minimally invasive treatment options which are safe and effective.
The HHT Foundation recommends that all patients and families with HHT be assessed at an HHT Treatment Center for proper screening and treatment. Due to the rarity and complexity of HHT, treatment requires coordination among multiple medical specialists. The UCSF HHT Center of Excellence includes team members from multiple subspecialties to provide a comprehensive approach to the screening, diagnosis, and treatment of HHT.
Referrals and Scheduling
To schedule an appointment, please call Interventional Radiology at (415) 353-8867, Monday-Friday, from 8am-4:30pm
Torianna Lomax
Patient Care Coordinator
Ph: (415) 353-8867
Fx: (415) 353-4503
Email: [email protected]
Please note that a referral may be required from your primary care physician depending on your type of health insurance.
If you are a physician referring a patient, please call Interventional Radiology at (415) 353-8867 or submit a referral to AMB REFERRAL TO HHT CENTER (REF340) in APeX.
Records may be faxed to (415) 353-4503 or mailed to:
UCSF HHT Center of Excellence
185 Berry Street, Suite 350, Lobby 6
Campus Box 0964
San Francisco, CA 94107-0946
Preparing for Your Appointment
In advance of your appointment, please be sure to:
- Mail or fax copies of any medical records related to HHT. These may include, but are not limited to, physician notes, genetic testing, laboratory reports, CT reports, MRI reports, ultrasound reports, cardiac study reports, endoscopy reports, colonoscopy reports, and operative reports. If you have questions about where to obtain any of these records, please call us at (415) 353-8867. If you are unable to send these records, please hand-carry them on the day of your appointment.
- Mail copies of X-rays, CT scans, and MRI scans (films or CD-ROMs) if they were performed someplace other than at UCSF. If you are unable to send these records, please hand-carry them on the day of your appointment.
- Bring completed HHT Center of Excellence New Patient Questionnaire Form (pdf).
- Bring a list of all your current medications, your insurance card and some identification that has your picture on it. If your physician gave you a written request for the appointment, bring that request form with you as well.
- Arrive 15 minutes prior to your appointment to check in and complete verify information with our reception staff.
If you are the parent or guardian of a child who will be visiting the UCSF HHT Center of Excellence, please be aware that many of the screening examinations require that the patient hold still for long periods of time. Special measures will be taken to ensure that your child remains comfortable and still to minimize the need for anesthesia.
More Resources
We invite you to visit the following websites for more information about the diagnosis and treatment of HHT:
HHT Foundation Website
Learn More About HHT Brochure (pdf)
Cure HHT Resource Library
HHT Guidelines
UCSF Neuroendovascular Surgery
If you have any questions about the UCSF HHT Center of Excellence, please call (415) 353-8867.
Torianna Lomax
Patient Care Coordinator
Ph: (415) 353-8867
Fx: (415) 353-4503
Email: [email protected]
Daniel Langston, NP
Clinical Coordinator
Ph: (415) 353-4872
Fx: (415) 353-4503
Email: [email protected]
Common Problems:
Nosebleeds
Telangiectasias in the nose, along with the nosebleeds they cause, are the most common sign of HHT. About 90 percent of people with HHT will ultimately develop recurrent nosebleeds by the time they reach their forties. The average age at which nosebleeds begin is 12, but they can begin as early as infancy, or as late as adulthood. The nosebleeds can be as infrequent as a few times a year or they can occur daily. When a nosebleed occurs, it can last anywhere from seconds to hours. The amount of blood lost may be one or two drops, or enough to require an emergency blood transfusion. Learn more (pdf)
Treatment
Often, nosebleeds can be successfully managed with lifestyle modifications including room humidification, topical moisturizers, and nasal rinses. When lifestyle modifications do not result in satisfactory reduction of nosebleeds, alternate options are available. An Otolaryngologist (ENT) can significantly improve the severity of nosebleeds with minimally-invasive treatments. Other treatment options include prescription nasal sprays, oral and IV medications, embolization, or surgical interventions.
Pulmonary Arteriovenous Malformations (PAVMs)
Approximately 40 percent of people with HHT have arteriovenous malformations in the lungs (pulmonary AVM or PAVM). People with HHT 1 (ENG) are five to ten times more likely to have PAVMs than those with HHT 2 (ACVRL1). PAVMs, particularly during pregnancy, have a risk of rupturing when blood volume tends to increase. This can be life-threatening. However, there are additional concerns about untreated PAVMs.
Normally, the lung arteries get smaller and smaller as they go deeper into the lungs, similar to the branches of a tree. At the ends of these artery branches, hair-like blood vessels called capillaries join the arteries and veins. These capillaries perform many important functions including allowing passage of oxygen into the blood as well as filtering the blood of impurities (clots, bacteria, air bubbles) before the blood circulates to the brain. With a PAVM, these capillaries are missing, and the artery connects directly to the vein. If the artery leading to the PAVM is larger than two to three millimeters in diameter, small blood clots can travel through the PAVM and go into the brain, causing a stroke. Bacteria can also travel through PAVMs and result in brain abscesses (a brain infection). Stroke and brain abscess can be life-threatening. Fortunately, PAVMs are almost always treatable with a procedure called pulmonary artery embolization. Learn more (pdf)
Screening
An echocardiogram with bubble study is the recommended test of choice for PAVM screening. This test uses ultrasound (sound waves) to determine if injected saline bubbles can get through the lung circulation and be seen back in the heart.
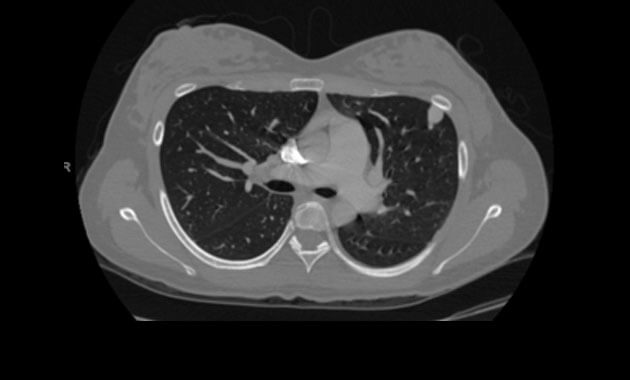
A chest CT scan may also be performed to evaluate for PAVMs. It is also highly sensitive for detection of pulmonary AVMs, but it involves radiation exposure. For this reason, a chest CT is usually reserved for those patients with known PAVMs or a positive echocardiogram with bubble study to determine if treatment is necessary and to determine the anatomy of the AVM and treatment options.
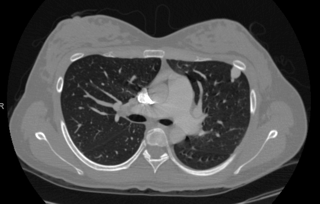
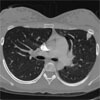
Chest CT depicting
Pulmonary Arteriovenous Malformations (PAVMs).
Treatment
A pulmonary angiogram and embolization is a minimally-invasive procedure performed by an interventional radiologist in an angiography suite. The patient is given sedation for this procedure. A catheter (a small tube) is inserted into an artery in the top of the thigh and directed through the body to the site where the embolization will be performed. An embolization coil is then injected through the catheter to block the blood flow through the AVM. After the procedure, the patient is transferred to the recovery area, where he or she is observed for several hours before being discharged home.
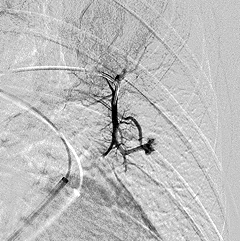
Pulmonary angiogram depicting
Pulmonary Arteriovenous Malformations (PAVMs).
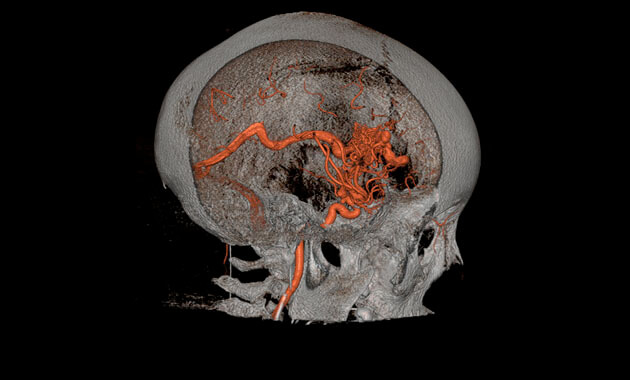
Brain Arteriovenous Malformations (AVMs)
Brain (or cerebral) AVMs are found in about five to twenty percent of people with HHT and can also be successfully treated in most cases. They can be life-threatening or disabling if they bleed. Since they often do not cause warning symptoms prior to bleeding, we recommend screening for them in all people with HHT, even infants. Other types of brain vascular malformations, such as capillary telangiectasias, cavernous malformations, and venous malformations, may be seen in HHT patients. It is not clear if these malformations are seen any more commonly in HHT patients than in patients without HHT, but they are less risky than AVMs and often do not require treatment. Learn more (pdf)
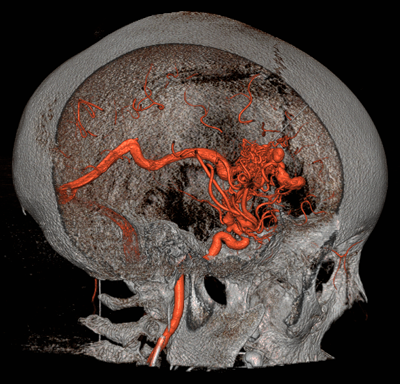
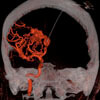
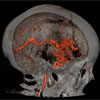
Brain Arteriovenous Malformations (AVMs).
Screening
Magnetic resonance imaging (MRI) of the brain is the recommended test for identifying cerebral AVMs. It utilizes strong magnetic fields to form images of the body. No radiation is used during this study. The duration of the procedure will vary, but the average is 60 minutes. The patient is required to lie still during the actual MR scanning. If the patient has claustrophobia, the doctor may prescribe an oral medication to bring along for the MRI appointment.
A cerebral angiogram is a minimally-invasive procedure performed by a neurointerventional radiologist in an angiography suite. The patient is given general anesthesia or conscious sedation for this procedure. A catheter (a small tube) is inserted into an artery in the top of the thigh and directed through the blood vessels in the body to arteries in the neck or the brain. The patient may require treatment, called an embolization, at the time of the procedure. After the diagnostic cerebral angiogram, if there is no embolization involved, the patient is transferred to a recovery area, where he or she is observed for several hours before being discharged home.
Treatment
A cerebral embolization is a minimally-invasive procedure performed by a neurointerventional radiologist in an angiography suite. The patient is given a general anesthesia for this procedure. A catheter (a small tube) is inserted into an artery in the top of the thigh and directed through the blood vessels of the body to the arteries in the neck or the brain. An embolization material is then injected through the catheter to treat the AVMs. This material could be small flexible coils, small plastic beads, or medical glues. After the procedure, the patient is transferred to the intensive care unit, where he or she is observed overnight before being discharged home unless the patient is then scheduled for additional surgery.
Gamma Knife treatment is a type of focused radiation that destroys the AVM tissue. This is sometimes done in lieu of or after embolization to ensure that the AVM is cured.
Gastrointestinal Bleeding
About 80 percent of those with HHT have telangiectasias in their stomach or intestines, but only 20 percent develop obvious gastrointestinal (GI) bleeding. The bleeding can range from mild to severe. Telangiectasias can be found anywhere in the gastrointestinal system, including the esophagus, stomach, small intestine, and colon (large intestine). Telangiectasias in the GI tract do not cause pain or discomfort. Symptoms of GI bleeding are black or bloody stools and/or anemia. Often patients do not notice any change in the stool but instead are found to be anemic through blood work. Anemia can cause fatigue, shortness of breath, chest pain, or lightheaded feelings. Learn more (pdf)
Screening
Esophagogastroduodenoscopy and/or colonoscopy are studies that utilize a thin, flexible, lighted viewing instrument (endoscope) to examine the inside of the digestive tract. The patient is given sedation and the instrument is inserted into the mouth (esophagogastroduodenoscopy) or the rectum (colonoscopy).
A capsule endoscopy is a large capsule containing a camera that is swallowed by the patient. As the capsule travels through the digestive tract, it takes photographs that are transmitted to a small receiver that is worn on the waist of the patient. The images can them be reviewed by the physician to identify telangiectasias. The capsule is passed through the stool during a bowel movement and is flushed away in the toilet.
Treatment
Telangiectasias that have been identified as a source of bleeding can be treated by cauterization (burning the area). Cauterization is performed during an esophagogastroduodenoscopy and/or colonoscopy.
Liver Arteriovenous Malformations (AVMs)
Liver AVMs are found in 32 to 74 percent of people with HHT, but they only cause symptoms in an estimated eight percent. AVMs in the liver occasionally cause heart failure, usually later in life. Heart failure can occur if the heart has been overworked for years, pumping extra blood through the low resistance pathway of a liver AVM (shunt), as well as through all the normal vessels of the body. There are several other even more rare and complex complications that can result when HHT affects the liver. Few physicians outside of clinics that specialize in HHT are familiar with these complications. Learn more (pdf)
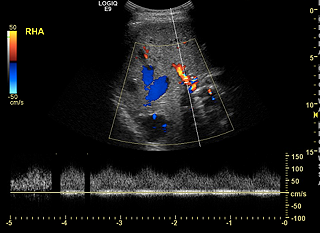
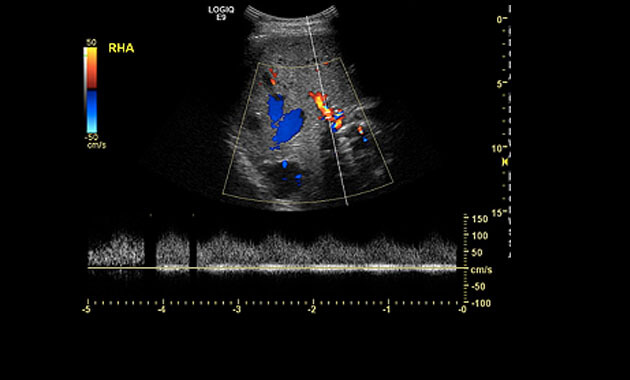
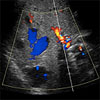
Ultrasound depicting a
Liver Arteriovenous Malformation (AVM).
Screening
A liver ultrasound uses reflected sound waves to produce a picture of the organs in the abdomen. No radiation is used during this study, and it is therefore the preferred method for screening liver AVMs.
An abdominal CT or MRI scan may also be performed to evaluate for liver AVMs.
Treatment
Liver AVMs rarely cause complications, and treatment is not recommended. Liver biopsies should also be avoided due to the risk of bleeding. Liver AVMs can result in elevated liver enzymes, which are usually not clinically significant. In rare cases, large or diffuse liver AVMs can result in heart failure. Those patients with significant liver AVMs should be followed routinely by a cardiologist.
HTT Center of Excellence Team
Because HHT symptoms can affect various parts of the body often early in a patient’s life, our team of specialists at the UCSF HHT Center of Excellence consists of experts in the fields of Interventional and Neurointerventional Radiology, Pediatrics, Medical Genetics, Hematology, Otolaryngology/Head and Neck Surgery, Cardiology, Gastroenterology, Neurology and Pulmonology.
HTT Interdisiplinary Team of Experts
- Mandar Aras, MD, PhD (Cardiology)
- Anna Butrymowicz, MD (Otolaryngology)
- Ilona Frieden, MD (Dermatology)
- Heather Fullerton, MD, MAS (Pediatric Neurology)
- Andrew Goldberg, MSCE, MD (Otolaryngology)
- Jose G Gurrola II, MD (Otolaryngology)
- Nerissa Ko, MD (Neurology)
- Jennifer C Lai, MD (Transplant Hepatology)
- Andrew Leavitt, MD (Hematology)
- Patricia Loftus, MD (Otolaryngology)
- R. Peter Lokken, MD (Interventional Radiology)
- Teresa De Marco, MD (Cardiology)
- Neil Mehta, MD (Medicine)
- Andrew Murr, MD (Otolaryngology)
- Najwa El-Nachef, MD (Gastroenterology)
- Kazim Narsinh, MD (Neurointerventional Radiology)
- Isaac Neuhaus, MD (Dermatologic Surgery)
- Michael Ohliger, MD, PhD (Radiology)
- Darcy Phelan, NP (Hematology)
- Steven Pletcher MD (Otolaryngology)
- Joseph Shieh, MD, PhD (Pediatrics and Medical Genetics)
- Mark Sugi, MD (Radiology)
- Thiennu Vu, MD, PhD (Pulmonology)
HHT Center of Excellence Co-Directors
The UCSF HHT Center of Excellence
Interventional Radiology Scheduling
(415) 353-8867
UCSF Imaging Center at China Basin
185 Berry Street, Suite 180, Lobby 6
San Francisco CA 94107
(Free validation for parking at this location)
Pediatric Patients
UCSF Ron Conway Family Gateway Medical Building,
5th Floor, Reception area 5A
UCSF Medical Center at Mission Bay
1825 Fourth Street
San Francisco, CA 94158
Patient Care Coordinator
Torianna Lomax
Phone: (415) 353-8867
Fax: (415) 353-4503
Email: [email protected]
Clinical Coordinator
Daniel Langston, NP
Ph: (415) 353-4872
Fx: (415) 353-4503
Email: [email protected]